The Rh blood group system is the most well-known system after the ABO system. When talking about blood types, most are familiar with the “positive” or “negative” that come after the ABO. That term refers to whether or not you possess the “D” antigen. The D antigen is only one part of the Rh system, which is among the most complex of the human blood groups, having over 50 antigens.
Molecular Structure of the Rh Antigen
To better understand the Rh system, let’s take a look at the structure. The antigen consists of proteins and is an integral part of the red cell membrane, weaving in and out of the membrane 12 times. Rh-positive individuals will have about 10,000-30,000 D antigens on each red cell.
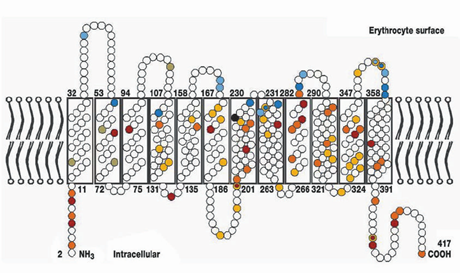
Until the late 1930s, only a few blood groups were known. There was evidence that other blood groups existed because even when ABO-specific blood was given, reactions still occurred. In 1939, Philip Levine and Rufus Stetson observed that a woman who had delivered a stillborn infant had a reaction when transfused with her husband’s blood, even though they were the same type (a common practice). They proposed that the reaction, as well as the cause of the infant’s death, was due to a factor in the blood of the husband and infant. When they tested the mother’s blood, she reacted with 80% of the people of her own blood group. This is consistent with the mother being Rh-negative and reacting with Rh-positive donors.
Over the next several years, other Rh antigens were identified, and several theories of inheritance and nomenclatures were proposed. We now know that Rh antigens are inherited on 2 genes, RHD and RHCE, located on chromosome 1. You inherit one gene from each parent. The D antigen is either present (Rh-positive), or absent (Rh-negative). The other major antigens are C, c, E, and e. These are codominant, meaning if you inherit C from one parent and c from the other, your red cells will express both antigens. The C and E antigens are also inherited together, as a group called a haplotype.
The Rh antigens are very immunogenic. Once a person is exposed to an Rh antigen they do not have, either through transfusion or pregnancy, they can easily form an antibody. Rh antibodies can cause severe reactions, so compatibility testing is vital if a person is known to have antibodies. Because of this, if a person is likely to need regular transfusions, facilities will match all of the common Rh antigens, not just the D antigen. This prevents the person from forming antibodies, which would make future transfusions difficult.
Variations of the D Antigen
To make the situation even more complicated, not all people are strictly Rh positive or negative. When tested by different antisera or different methods, some people were found to have varying reactions. Some individuals do not react with anti-D unless an indirect antiglobulin test is done. This was originally referred to as “Du”. Some individuals made anti-D while others did not.
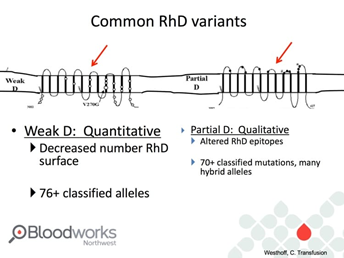
With the availability of molecular testing, it is now known that there are 2 groups: weak and partial D.
Some possess the D antigen but with very few antigen sites. Changes to the structure inside the cell or membrane result in weakened expression. Because they possess the D antigen, they do not make anti-D and can be considered Rh-positive.
Partial D individuals are missing part of the antigen, or have an altered form. These are changes to the structure outside the cell membrane. These people can make anti-D if exposed to Rh-positive blood and should be considered Rh-negative if getting a transfusion or if pregnant. However, they are considered Rh-positive if donating blood.
In Conclusion
The Rh system is significant in many ways, from transfusion reactions to pregnancy complications. In addition to the 50 known antigens, there are a large number of variants, most of which can only be identified through molecular testing. After over 80 years of research, we still have much to learn.

